PROJECT
Providence, Saint John’s Health Center – New Campus, OR Lights
PROJECT TYPE:
Acute Care Hospitals
LOCATION:
Santa Monica, CA
COMPLETION:
April 2020
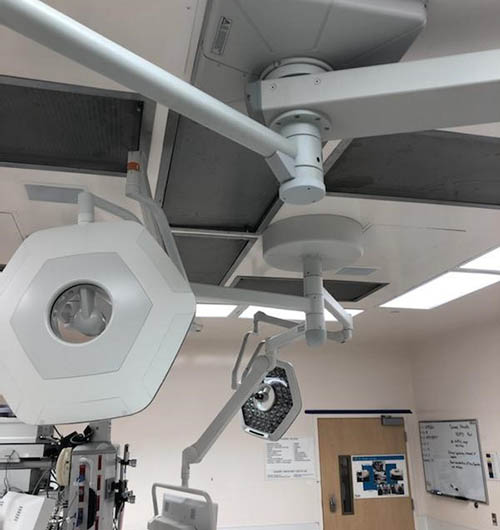
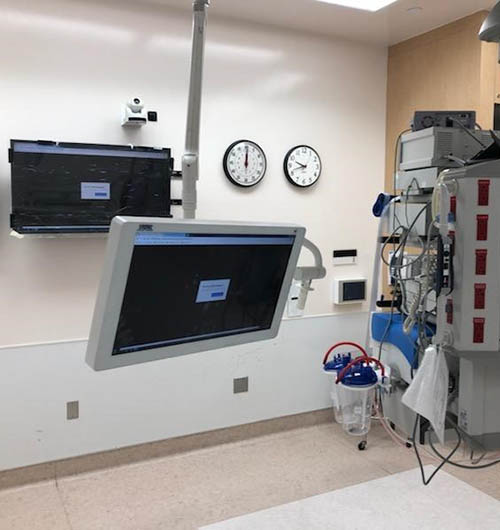
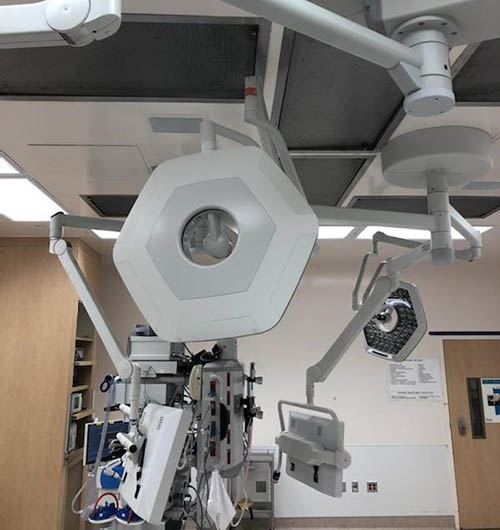
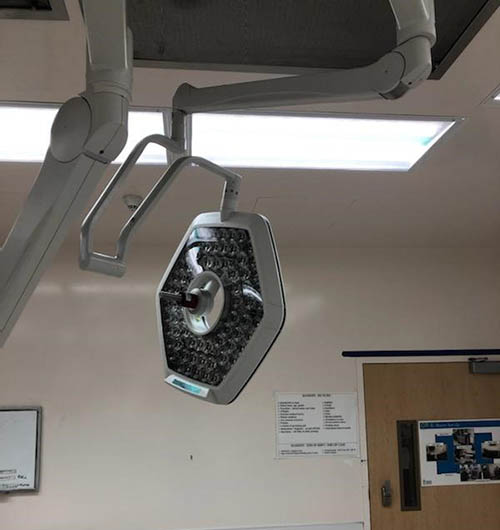
OR Lights Fast-Tracked
In November of 2019, Stahl was invited by Providence to lead the effort to install new lights & monitors in 12 operating rooms at Saint John’s Health Center, Santa Monica, California. Early on, the project was reduced to 10 OR’s with an expected time for construction to be four to six weeks. Through coordination with the design team, users, contractors, equipment vendors, OSHPD, and IORs we were able to start the installation four days from receiving the Building Permit. We proceeded to complete the installation in 10 days, down from the planned 4 to 6 weeks along with the increase from 10 to 11 ORs.
While reducing the project duration time by more than 70% was a feat in and of itself, it was perhaps the overcoming of obstacles along the way that made this so impressive.
These obstacles started with a misunderstanding, due to new accounting practices, which led to a mix-up with payment and a delay in issuing the building permit. After two weeks, AP finally adjusted and made an emergency check run to make payment for issuance of the building permit.
Then, a capital freeze went into place a day prior to commencing construction. This was meant to conserve cash to be able to address the coronavirus pandemic. The team rallied alongside hospital leadership working with the region and Providence system to get funding released from the freeze. This project was deemed Essential for patient and caregiver safety.
Getting the ICRA permit signed off by the epidemiologist, for construction to start, became the next obstacle. The hospital was so involved dealing with the preparations for COVID-19 Pandemic Preparedness that availability was all but impossible. Again, the team rallied. This time it was nursing staff who hunted down the necessary signature to finalize the permit and allow construction to begin.
Weekend Work Facilitated Result of Cancelled Surgeries
The department didn’t want to have any more than one room unavailable for surgeries at any given time and preferred work be done over weekends. We saw an opportunity with the recently canceled elective surgical cases (due to COVID-19) to make a run at two rooms per day. Once the work commenced, it became clear that work during the day was becoming difficult intermixing with nursing operations. Again, the team rallied and changed to working at night. Nursing saw the speed and ease with which our coordination allowed the team to move and opted to keep us working throughout the weekdays and through the weekend.
The next challenge came with the OSHPD Compliance Officer being on a two-week schedule to visit the campus and wanting to see the first installation prior to allowing the operating room to be used for surgeries and prior to proceeding with the next room. Worse, his next site visit fell on a holiday which he had coupled with another day off. At best, we would need to wait at least four days to see him. Working with OSHPD, we were able to negotiate typical IOR inspections, followed by verified compliance reports being issued by the design professionals prior to re-occupying the room and only needing the Compliance Officer to validate via photos and shared paperwork, at a later date.
In the end, we were able to return 11 rooms back into circulation in just 10 days, while overcoming the final obstacle of allowing four of the rooms to be made ready for potential COVID-19 patients by creating temporary negative isolation rooms for surge readiness.